
Breast Cancer Procedures
Anne Peled, M.D., is acclaimed as one of the best oncologic and plastic surgeons in San Francisco, California, and is widely recognized for her unique dual training in both breast cancer and reconstructive surgery. What this means is that you will have one surgeon for both your breast cancer surgery and your reconstruction, which often limits the duration and number of procedures. This also means that you will have access to Dr. Peled's cutting-edge techniques through your whole course of treatment, from mastectomies where she preserves sensation in the breast and nipple, to thoughtfully-planned incisions where she is able to hide and minimize scarring.

Breast Biopsy
Breast biopsy involves removal of a small amount of breast tissue to help get more information about a breast mass or abnormality seen on breast imaging or exam. This is an outpatient surgery with typical recovery lasting one week. Once the pathology is reviewed from the surgery, next steps in treatment (if needed) can be decided.
Lumpectomy
Based on certain characteristics of a woman’s breast cancer, she may be a candidate for lumpectomy, where the known cancer is removed surgically in addition to a margin of normal tissue around the cancer. Depending on the situation, lumpectomy may be done with axillary lymph node biopsy, which involves removal of some of the lymph nodes under the arm to assess for cancer. Lumpectomy is ideally performed with scars hidden to minimize any visual reminder of the surgery, and in conjunction with reconstruction, where the breast tissue is reshaped at the time of lumpectomy to make the breast shape look more normal. Sometimes this reshaping involves either a breast reduction or a breast lift, which is often done in both breasts so the breasts look symmetric. Reconstruction at the time of lumpectomy is often called "oncoplastic reconstruction."
Oncoplastic reconstruction for lumpectomy
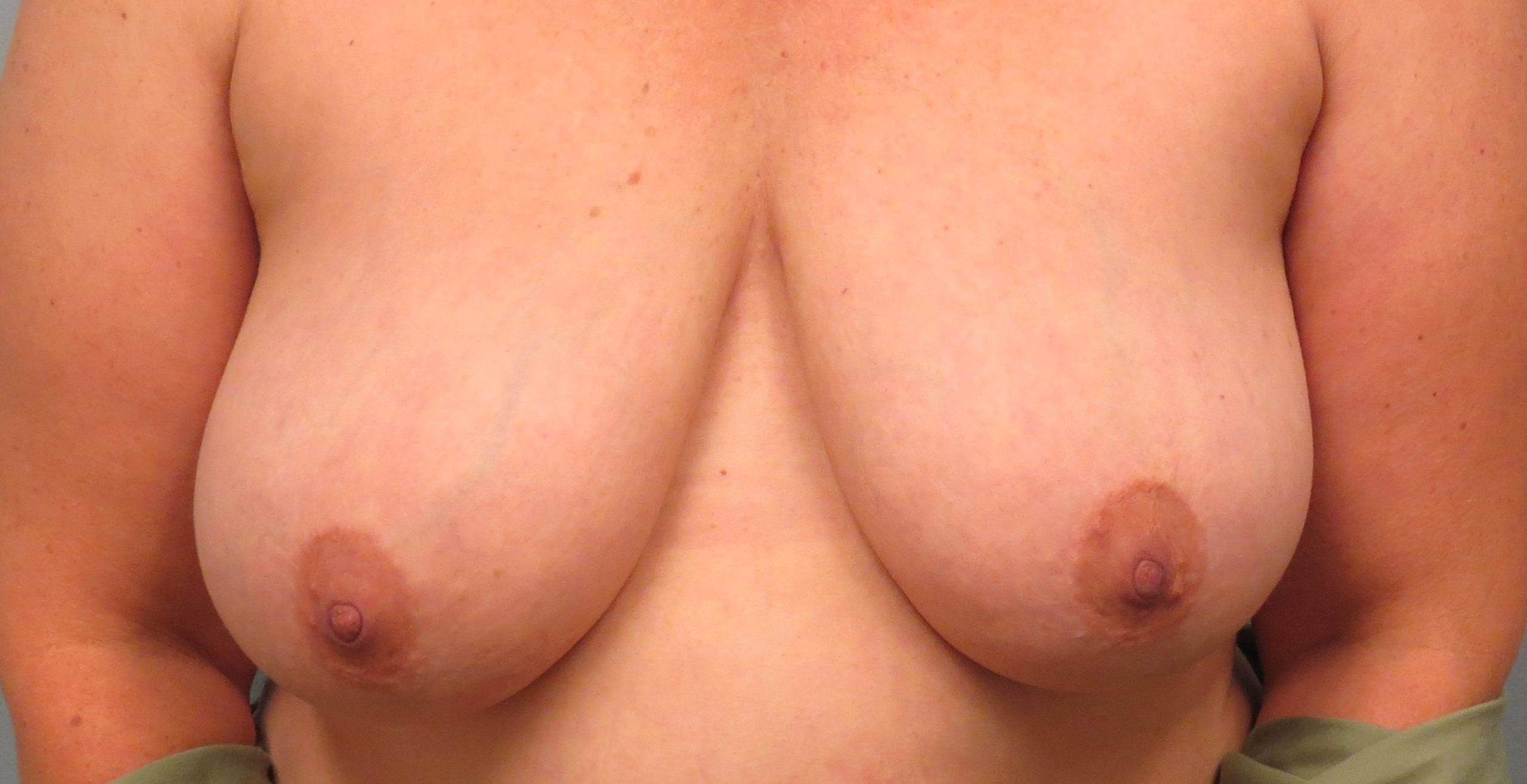
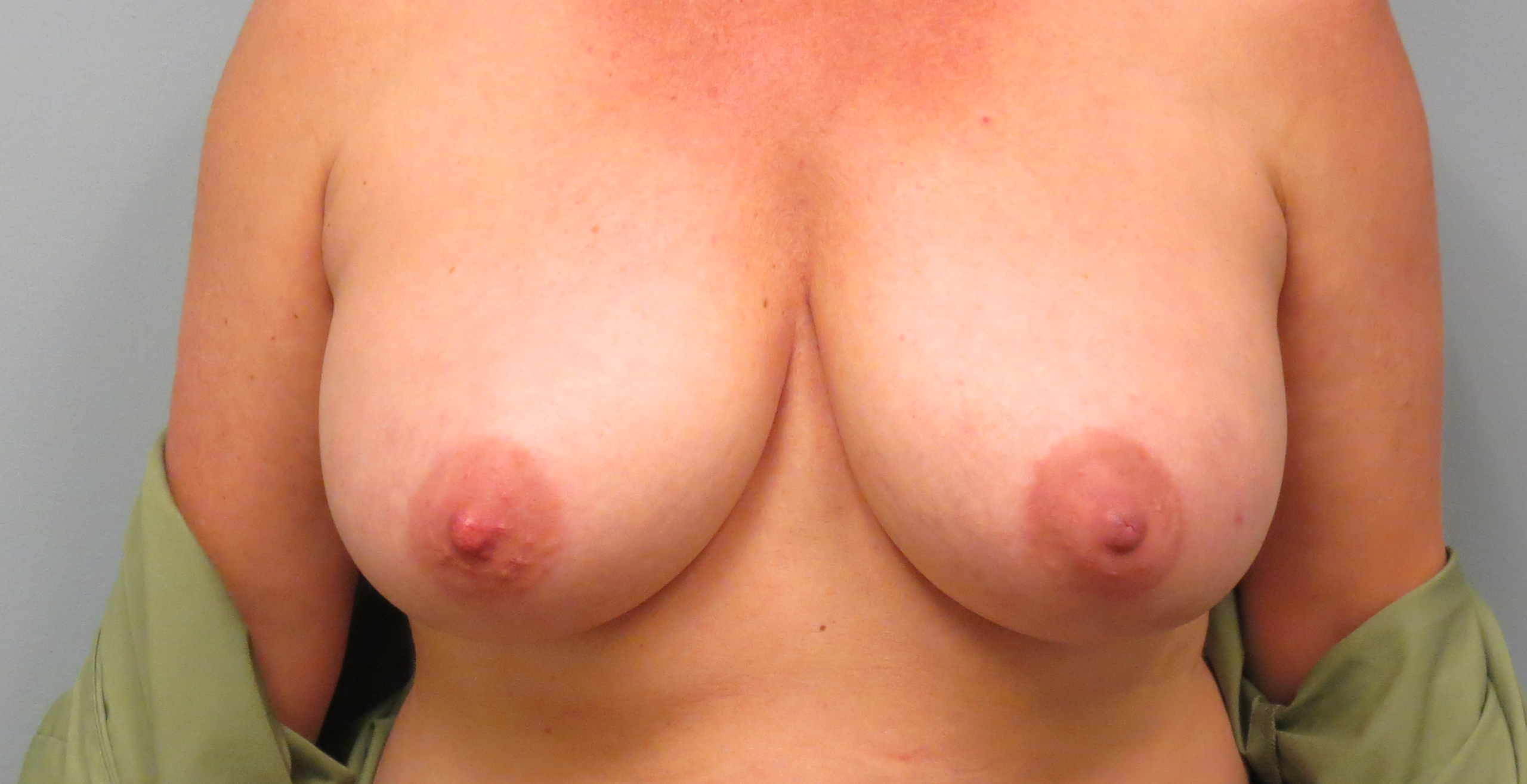
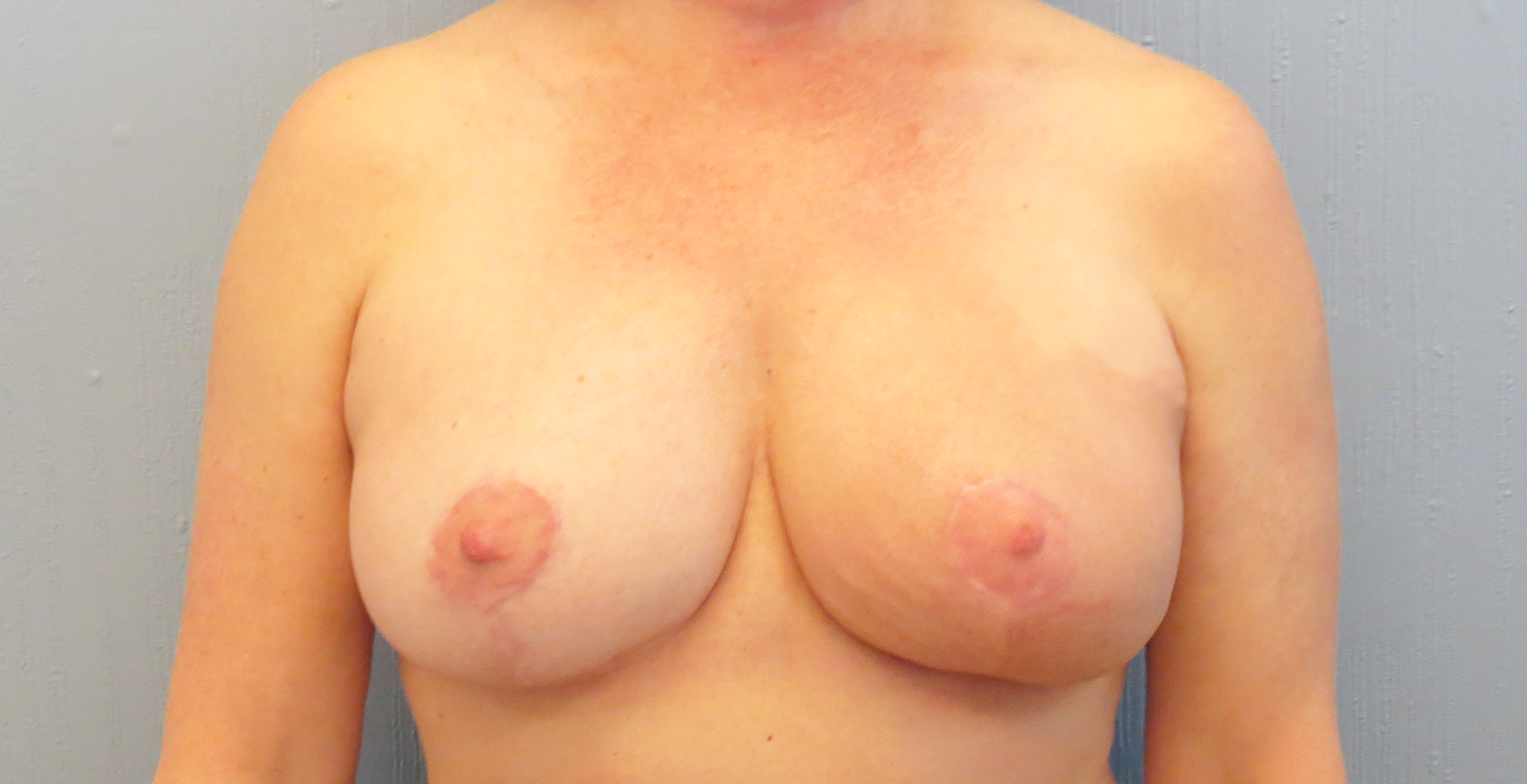
Oncoplastic surgery is the term used to describe reconstructing the breast tissue at the time of lumpectomy to help improve the appearance of the breast after surgery. This can be done in many different ways, with the ultimate goal to fill the defect left after the lumpectomy so that there is not a deformity in the breast after surgery. One type of oncoplastic surgery involves rearranging and moving breast tissue after the lumpectomy is done to fill in the space using the same incision made for the lumpectomy. Another technique involves doing a breast lift, which allows for entails typical breast lift incisions around the nipple and sometimes on the lower part of the breast, which allows for improved rearrangement and reshaping of the breast to fill the lumpectomy defect. An additional option for larger-breasted women is doing a breast reduction at the time of lumpectomy, which includes removal of the breast tissue needed for lumpectomy, as well as other breast tissue and skin, to help reshape the breasts, fill the lumpectomy defect, and make the overall breast smaller and more lifted. When breast lifts or reductions are performed, a similar procedure is usually done on the opposite breast so that the breasts match after surgery. While these techniques do make the surgery time, and sometimes the recovery time, slightly longer, they are great options for women to help them get the best breast appearance following surgery. In many cases, women’s breasts appear even better than they did before surgery.
Oncoplastic Reconstruction Before and After



Lymph node biopsy
One of the most important factors influencing treatment plans and overall prognosis for breast cancer is the tumor stage. Tumor stage is related to how large the tumor is, as well as whether or not it has spread to other parts of the body, such as the regional lymph nodes. The primary lymph nodes draining the breast are found in the armpit (also known as the axilla). In order to see if the cancer has spread from the breast to the axilla, a surgical biopsy of a small number of axillary lymph nodes can be done at the time of lumpectomy or mastectomy. In certain cases where the lymph nodes are known to be involved with cancer before surgery, removal of a larger number of lymph nodes at the time of lumpectomy or mastectomy will likely be recommended to help with tumor staging and prevent the cancer from coming back in the area.
HIDDEN SCAR
Studies show that scars from breast cancer surgery can impact a woman’s self-confidence, intimacy, and body image, making the cosmetic outcome equally important as removing cancer (or risk of cancer). However, many physicians, although trained in cancer removal, do not have the advanced training on removing breast cancer (or the risk of breast cancer) while placing an incision in a location that is hard to see. With a Hidden Scar approach, your incision is placed in a location that is hard to see, so your scar is not visible when it heals. Women who decide Hidden Scar is right for them do not have a higher risk of cancer recurrence than patients who undergo a traditional technique. Click here to read more.
Nipple-Sparing Mastectomy
A mastectomy may be recommended in several different situations, such as patients with certain breast cancer characteristics or women at high risk for developing breast cancer in the future. Depending on the situation, a mastectomy may be done with axillary lymph node dissection, which involves removal of some of the lymph nodes under the arm to assess for cancer. Although in the past, mastectomies used to involve removal of most of the chest skin and even the chest muscles, current mastectomy techniques are much less invasive. Most mastectomies performed are either skin-sparing, where all of the breast skin except for the nipple and areola is saved, or nipple-sparing, where all of the breast skin including the nipple and areola skin is saved. When performed with breast reconstruction, these approaches can help make the reconstructed breast look more natural and more like the breast before mastectomy.
There are four common incision types for Nipple-Sparing Mastectomy, which allow scars to heal well and fade over 6-12 months: inframammary fold (underneath the breast), peri-areolar (around part of the areola), lateral (from the side of the areola out towards the side of the breast), and inferior vertical (from the bottom of the areola down towards the bottom of the breast).


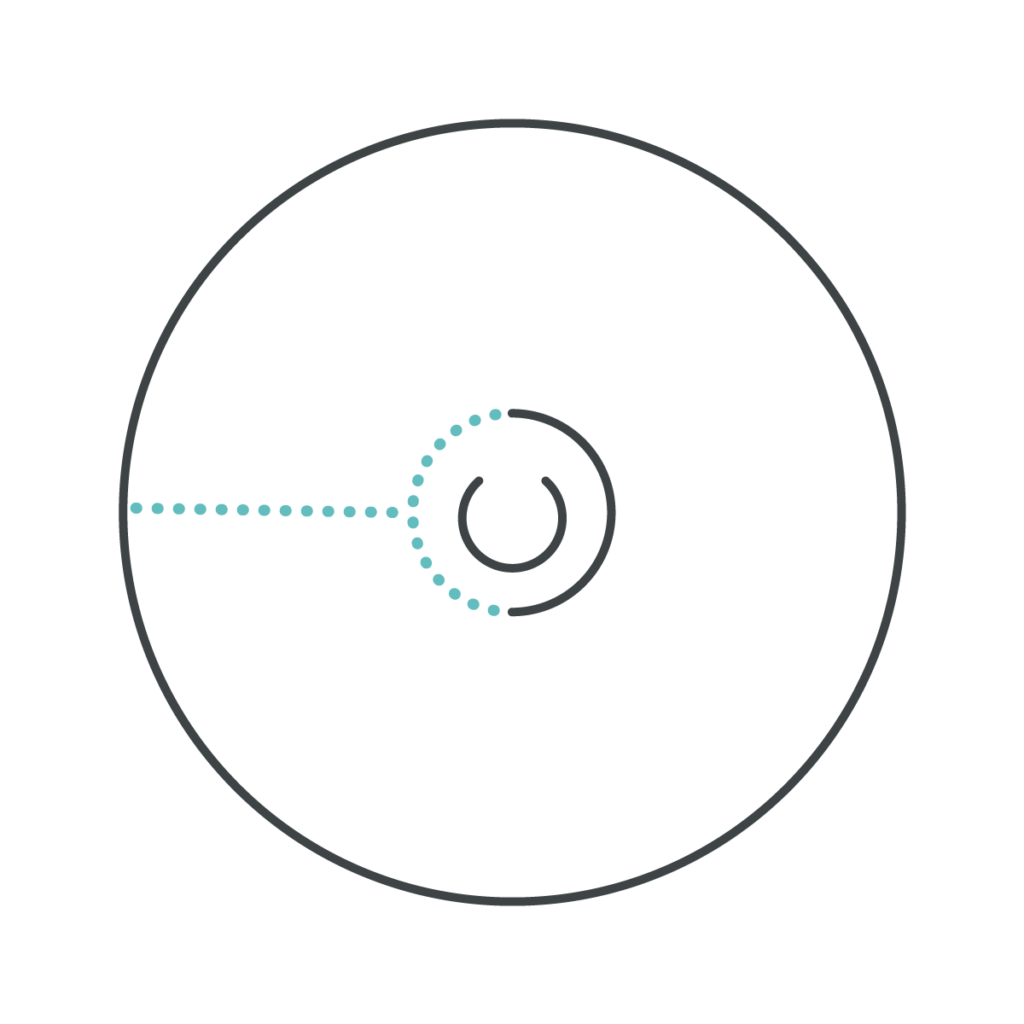

Nipple-sparing MASTECTOMY
BEFORE & AFTER
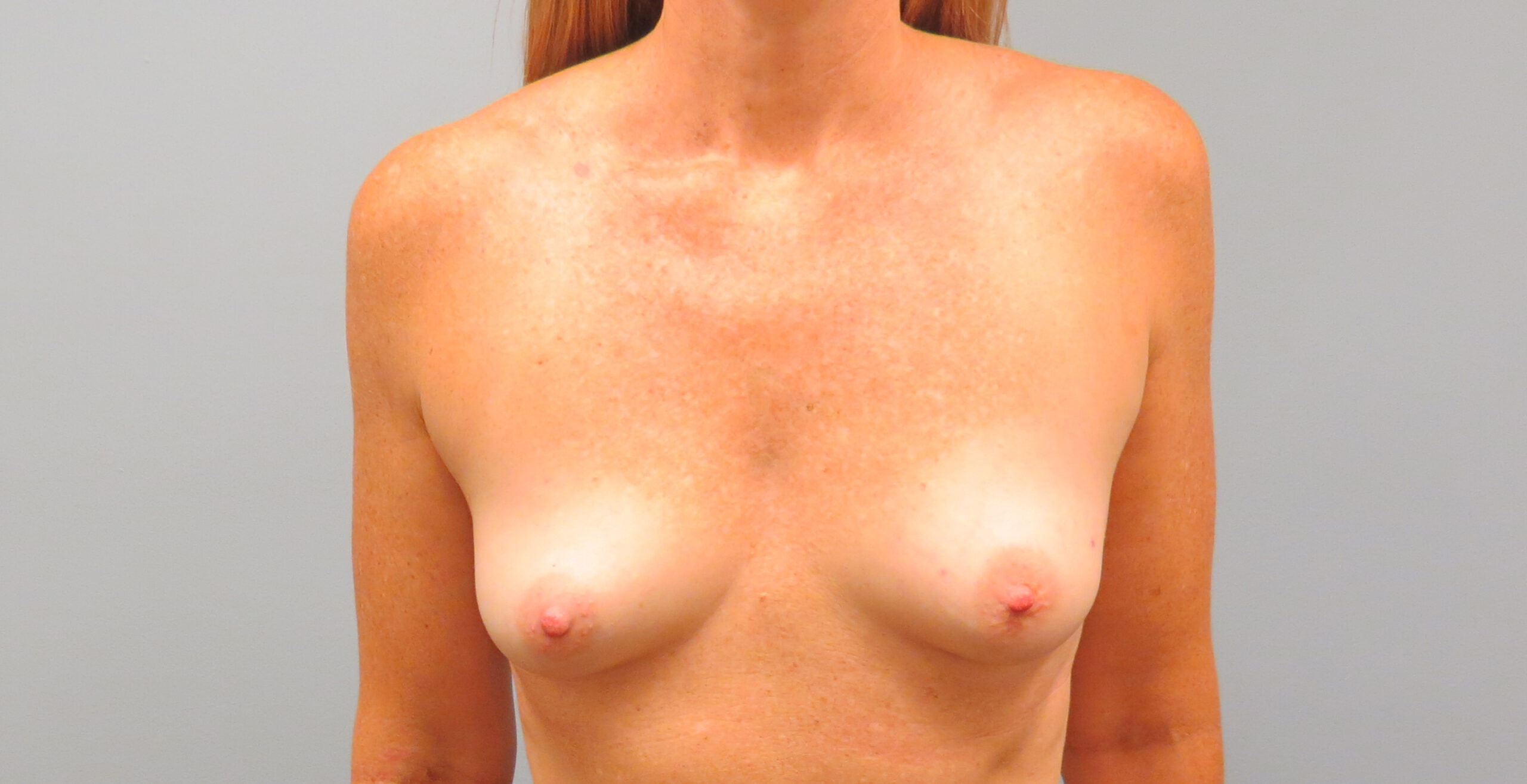

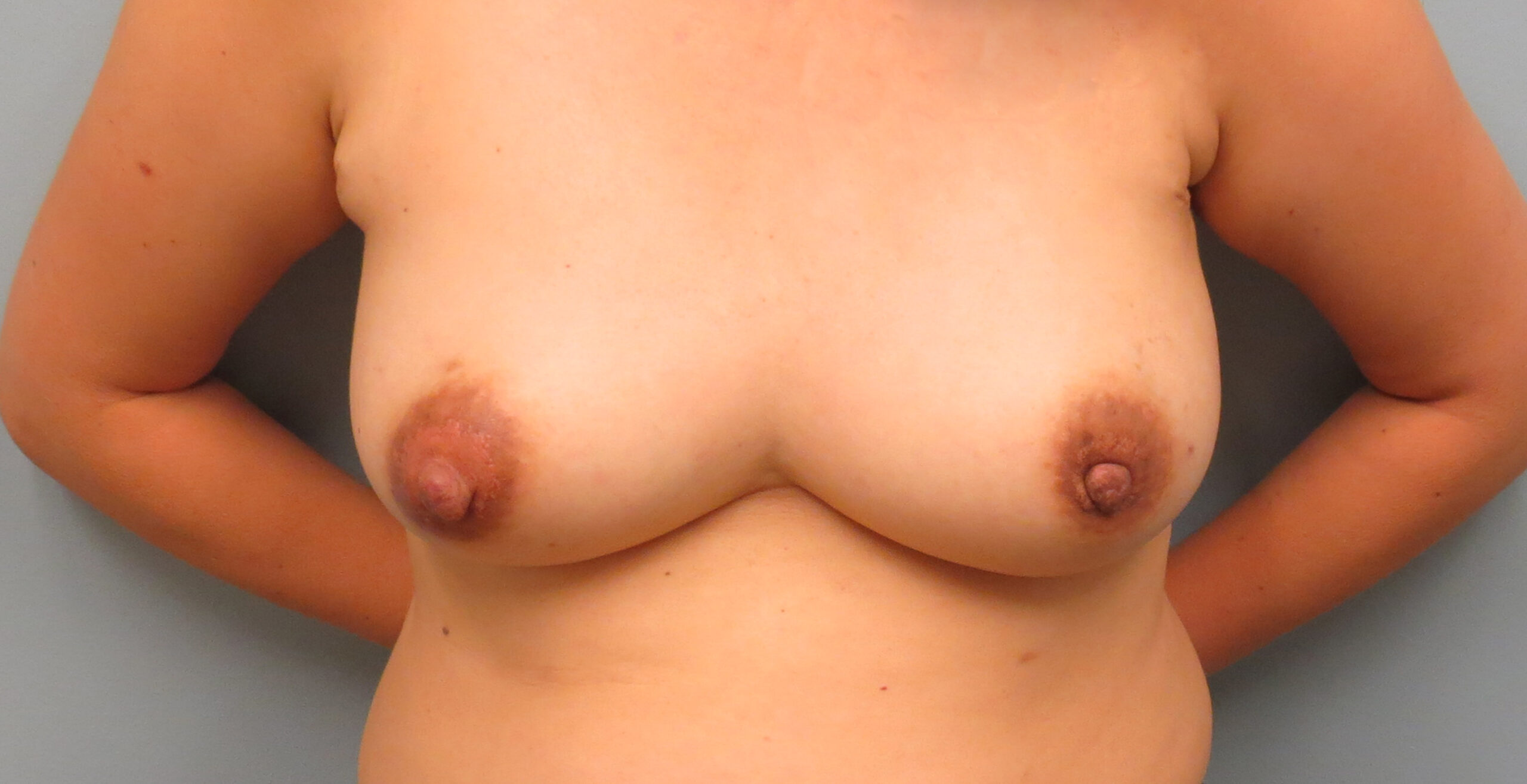
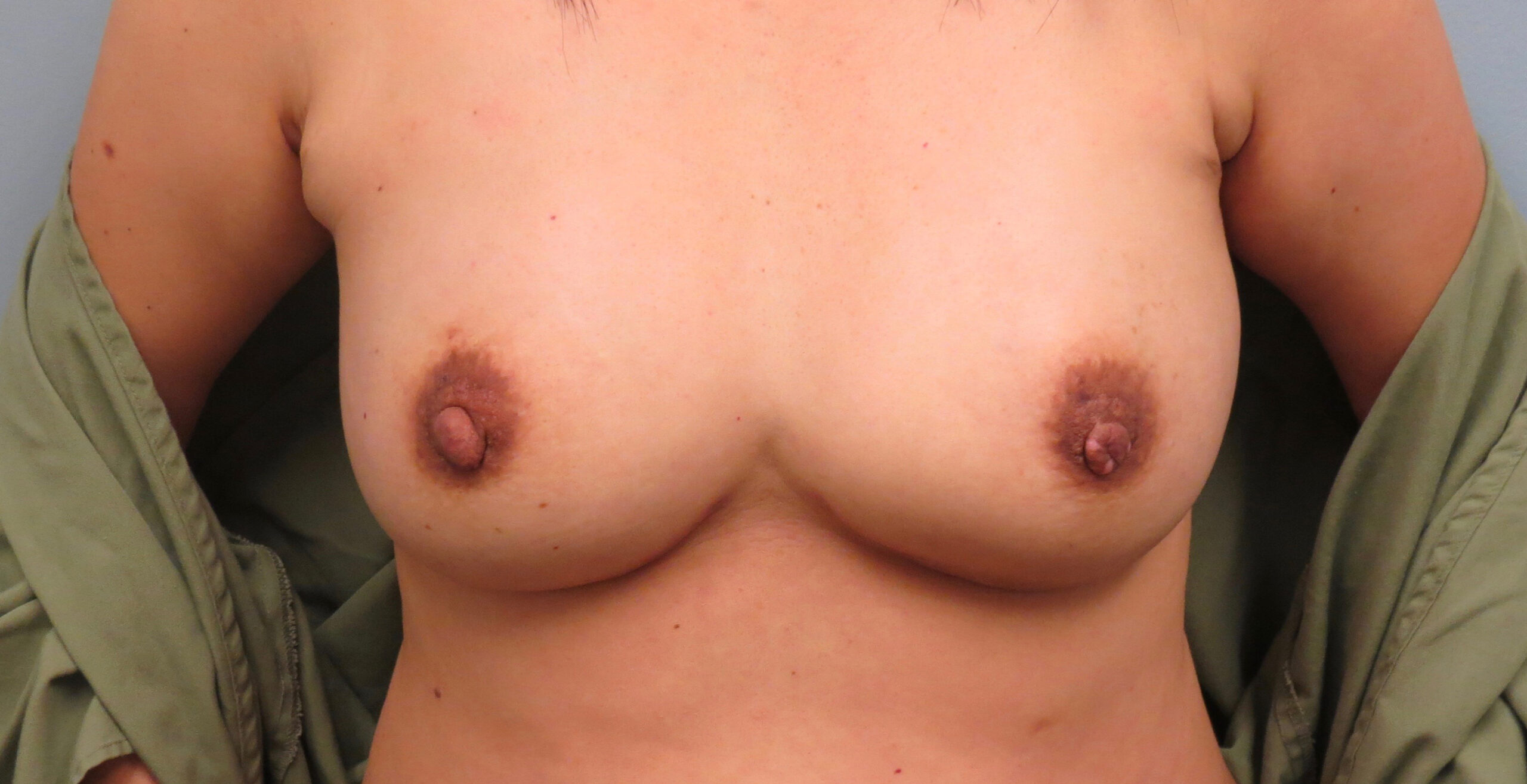

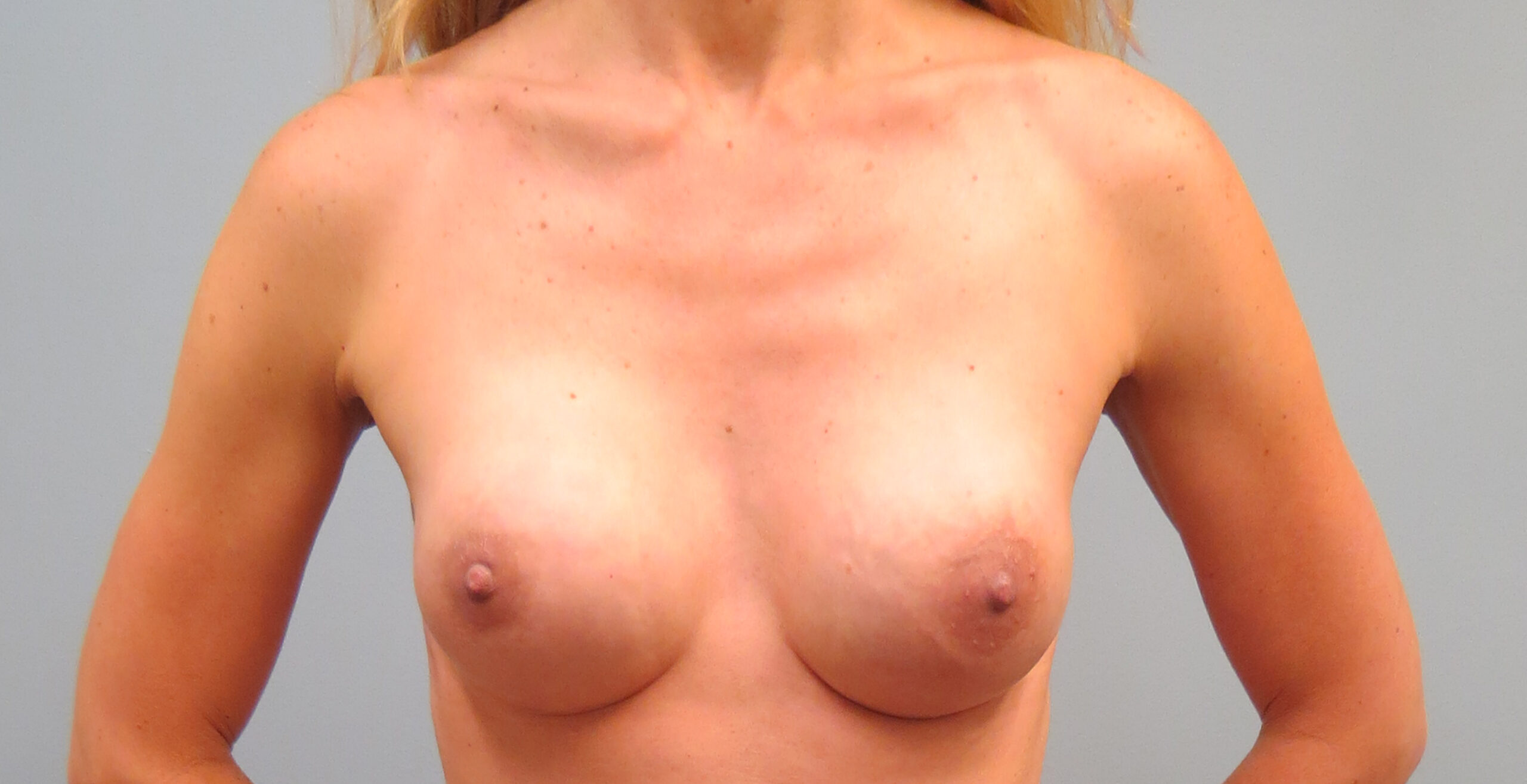
sensation-preserving mastectomy
Traditional mastectomies (because of the way the nerves in the breast skin and nipple travel through the breast tissue) tend to cut through the nerves, which leads to breast skin and nipple numbness for many women, or or even sometimes painful sensations at the cut nerve ends. To try to prevent this numbness or pain, Anne Peled, M.D., a breast oncology and reconstructive surgeon, and Dr. Ziv Peled, a peripheral nerve and plastic surgeon have been doing nipple-sparing mastectomies, where they carefully preserve the nerves during nipple-sparing mastectomies and/or do nerve grafting if nerves cannot be preserved safely. They have done a number of these mastectomies combined with immediate implant reconstruction and most women report that their breasts feel almost the same or exactly the same as they did before surgery. To learn more about sensation-preserving mastectomies and click here.
Implant-based reconstruction
Common options for breast reconstruction after mastectomy include implant-based reconstruction and autologous reconstruction using a woman’s own tissue. Implant-based reconstruction for mastectomy can be done in either one stage, where a permanent implant is placed at the time of mastectomy, or in two stages, where a temporary implant called an expander is placed at the first stage and switched to a permanent implant at the second stage. The decision on which approach to use is based on pre-mastectomy breast size and shape, patient goals, and intra-operative assessment following mastectomy. The main benefit of implant-based reconstruction is that no large additional scars outside of the breast are needed and the post-operative recovery is often easier, with a typical two-week recovery period. Implant-based reconstruction frequently includes fat grafting at the second stage of reconstruction in order to help give the most natural appearance of the breast following reconstruction.
Direct-to-Implant Reconstruction
As implant-based breast reconstruction has evolved, two-stage reconstruction with an initial expander is no longer is often no longer necessary. Many plastic surgeons are now realizing that selected patients may be able to have one-stage surgery with an implant placed at the time of mastectomy, which is known as direct-to-implant reconstruction or a "One and Done” approach. The benefits of this approach are that women can avoid the need for a second surgery for the exchange and get to their final reconstructive outcome more quickly.
choosing YOUR IMPLANT TYPE
When you choose implant reconstruction, you can have implants that are filled with silicone or saline. Silicone implants are chosen more often because they are softer, lighter, durable, have more natural look, and are less likely to ripple. They also have a range of "gumminess," which informs the durability and shape of the implant.
OVER OR UNDER THE MUSCLE
Pros: Patients can have a more natural-appearing upper part of the breast, less chronic pain and functional issues from cutting and disconnecting the pectoralis muscle. Patients who have had prior radiation or are expected to have post-mastectomy radiation will also be able to have better shape and symmetry with over-the-muscle implants.
Cons: With over-the-muscle implants, patients may potentially experience more rippling along the top of the breast, and mastectomy skin flap irregularities can be more visible. In addition, some surgeons may not offer this technique depending on their experience and training.
Pros: Under-the-muscle implants are a more familiar technique for many surgeons, based on their prior training. Patients are less likely to have rippling or visible edges of the implant along the top of the breast, and potentially can have better screening for future recurrence if the cancer is right on top of the chest muscle.
Cons: With under-the-muscle implants, patients can experience more short- and long-term pain, and frequently have “hyperanimation deformity” along the top of the breast with pectoralis movement. In addition, the implants are often displaced towards the armpits/sides or appear flattened along the top.
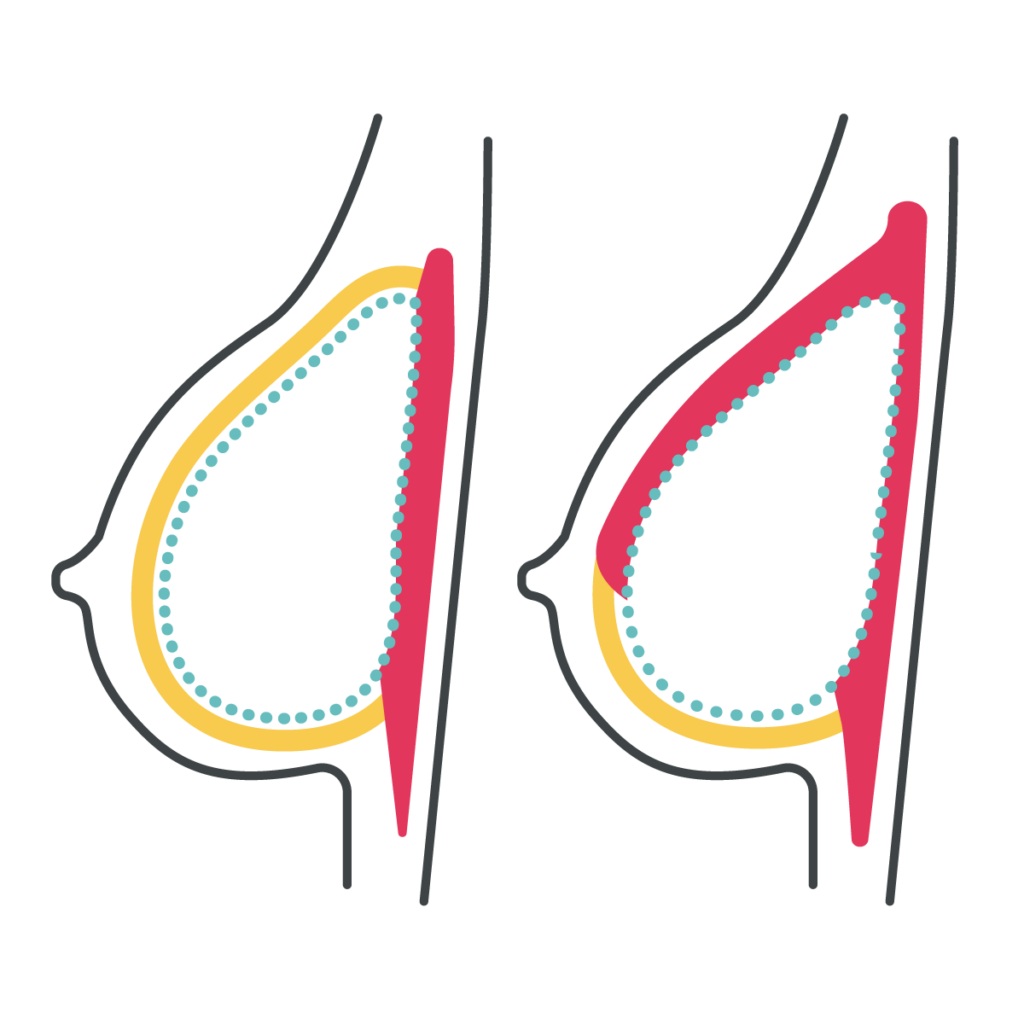
Flap RECONSTRUCTION
Reconstruction using a patient’s own tissue can be done with tissue from many different parts of the body, including the abdomen, thighs, buttocks, or back. The technique used depends on several factors, including the amount of available tissue in the potential donor area, patient preference, the amount of breast tissue needed for reconstruction, and other factors in the patient’s medical history or breast cancer treatment plan. Flap reconstruction can allow for a natural appearing breast reconstruction, as the reconstructed breast feels and looks like similar to breast tissue. Flap reconstruction does involve making additional scars outside of the breast in order to move tissue from the selected donor site to the breasts.
Flap Reconstruction before & After
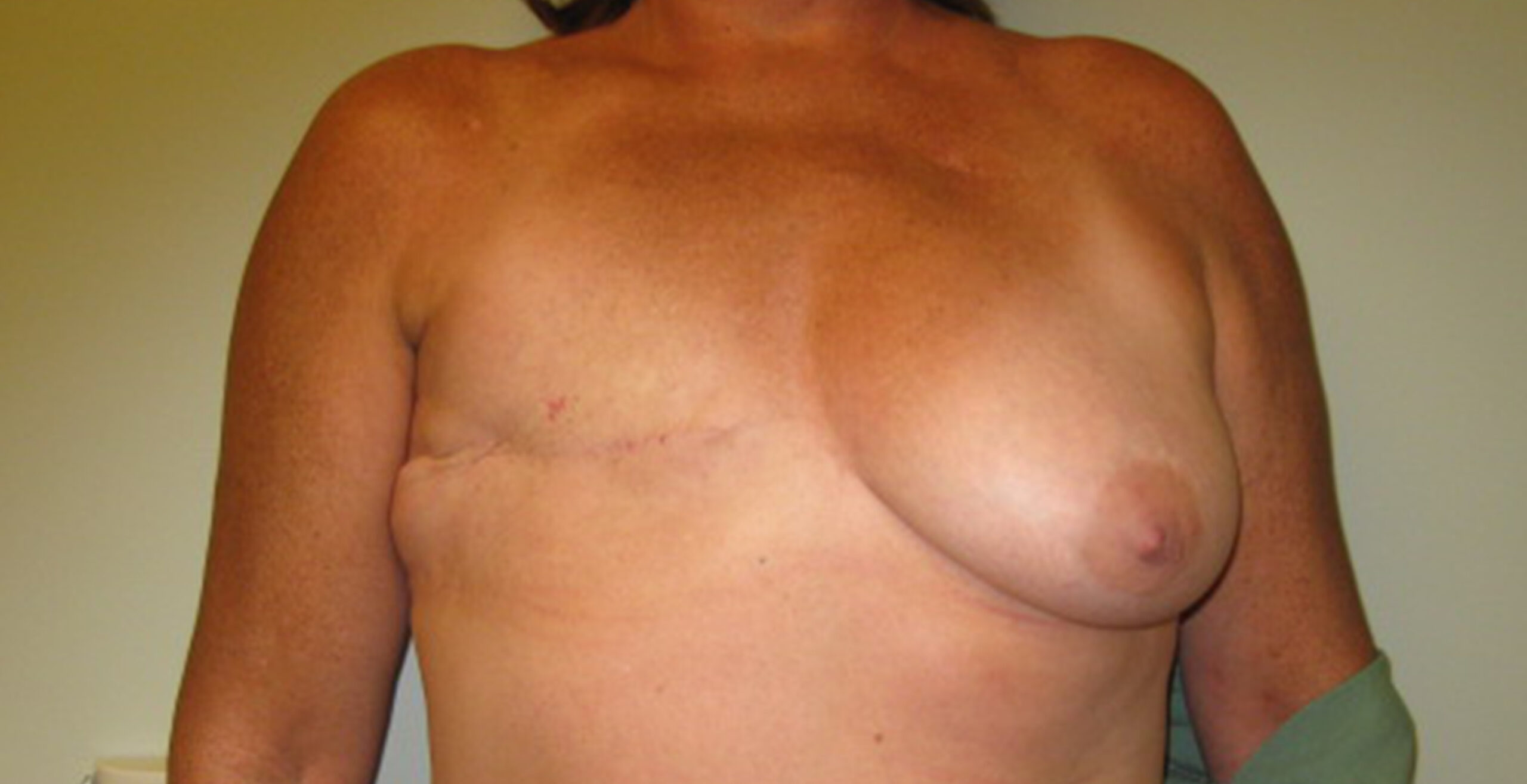
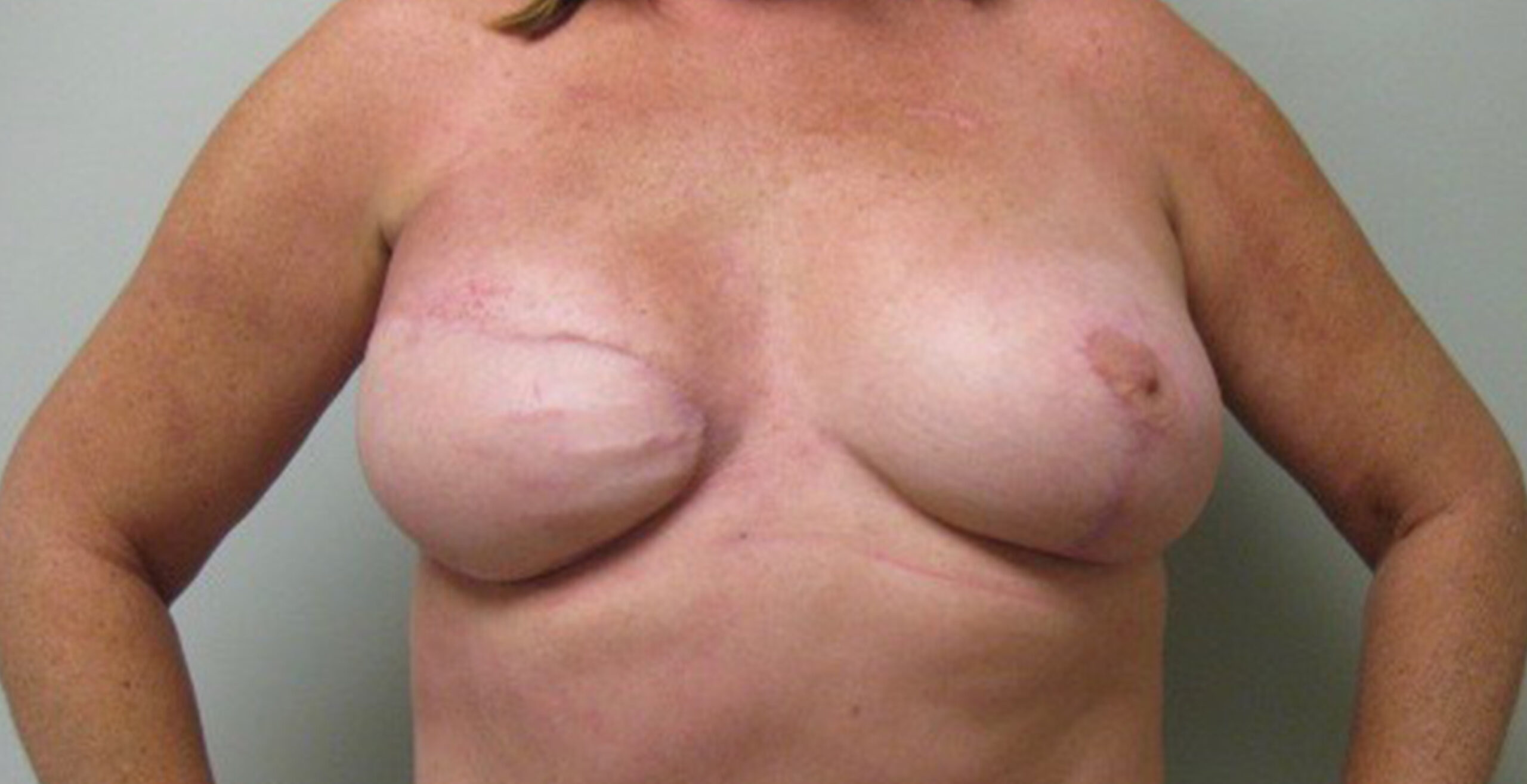





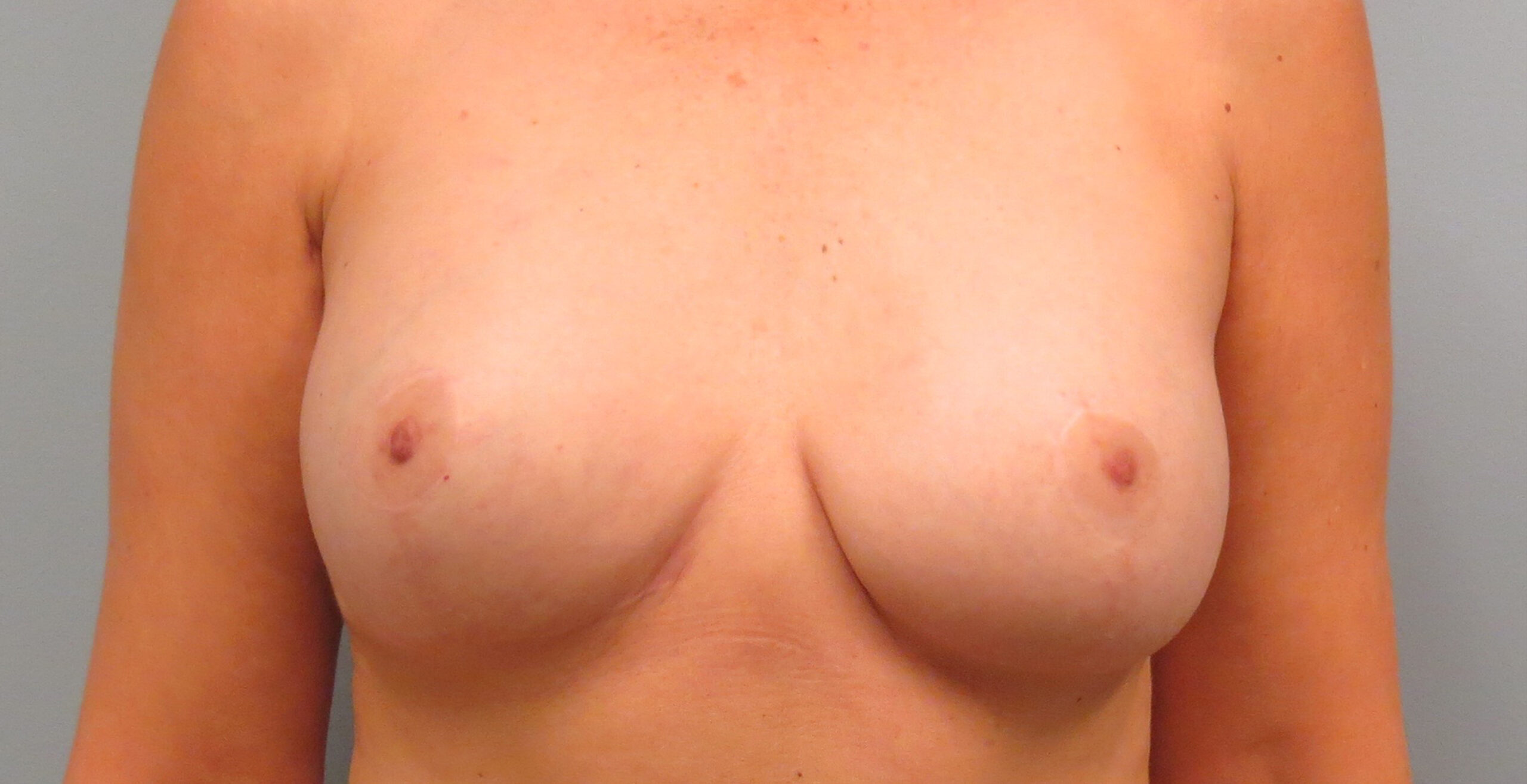


Fat Grafting
Fat grafting can be done as a part of reconstruction following lumpectomy or for post-mastectomy reconstruction, either implant-based or flap reconstruction. The typical reason fat grafting is used after lumpectomy is to fill defects in the breast after lumpectomy, which can become more apparent following radiation therapy. Reconstruction with fat grafting can be done any time after lumpectomy, though it is best to wait at least six months to 1 year following radiation therapy in order for the breast to be completely healed from the radiation effects. When fat grafting is used for post-mastectomy reconstruction, it is typically done as part of the second stage of reconstruction, where fat is injected throughout the mastectomy skin flap and sometimes the chest wall muscles to help increase the size of the reconstructed breast and make the shape appear more natural. In both cases, fat grafting entails standard liposuction (typically of the abdomen and/or thighs) in order to obtain fat to use for the reconstruction. The fat is then specially processed in the operating room to get it ready for transfer. After that, it's carefully transferred back to the breast or mastectomy skin flaps in small amounts throughout the area to prevent lumpy areas within the breast (“fat necrosis”).
Common QUESTIONS
Depending on the procedure, recovery time can be any time from 4 to 6 weeks.
You can usually start walking within the first week, and can then slowly increase your exercise over next several weeks. You are generally back to full activity in 4 to 6 weeks.
You can view our favorite post-surgical products here.
Legally, insurance companies are required to cover breast cancer and breast recon procedures, but patients will need to verify this with their individual insurance providers before their surgery.
Older generation implants are thought to only last 10 years, but they are anticipating that newer ones will last from 20 to 25 years.
It’s best to speak with a physician to determine which procedure is the best for you.
Saline and silicone implants have different benefits depending on the patient. Newer silicone gel implants (a.k.a. “gummy implants”) are commonly used when silicone is selected.
Most women receive smooth implants, but this is always a personalized discussion with each patient.
Breast feeding can be impacted by any type of breast surgery, but there are many women who are able to successfully breast feed after certain types of breast cancer procedures. If you are undergoing a mastectomy, however, you will not be able to breast feed.
Our office has a scar management system that is customized for each patient.
Most people take 1 to 2 weeks off after surgery before they return to work, although that period can be longer if patients have additional/combined procedures involving different parts of their body.
Depending on the breast cancer procedure, varying levels of loss of sensation can occur. This is exactly why Dr. Peled has developed a new “sensation preserving mastectomy” technique, in order to preserve breast sensation during mastectomies and reconstruction. Click here to learn more.

